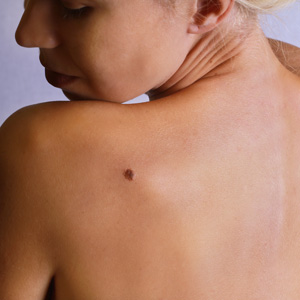
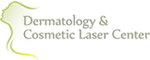Many people have moles, technically called nevi, from the time they are born. Many more develop new moles, or acquired nevi, as they go through life.
Acquired Nevi
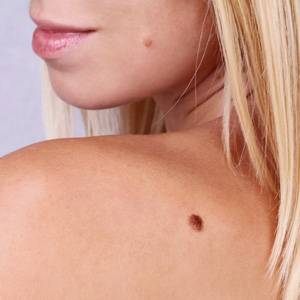
Moles that are not present at birth are thought to be mostly the result of sun exposure, although genetics also plays a role. Acquired moles may develop at any time, from childhood to well after mid-life. Usually, an acquired mole, which may grow alone or in a group, will grow no larger than ¼ inch. Though moles are typically thought to be dark brown spots, the truth is a mole may be flesh-toned, pink, brown, black, or some other color. A mole may be raised or flat, and may have hairs growing from it. Hair growth from a mole does not necessarily indicate abnormality.
Moles may develop on any area of the body. A normal mole may become darker, especially after sun exposure or during pregnancy. Some moles may darken as a result of certain medications or as a sign of cancerous change. In a normal mole, the risk of melanoma is relatively low.
Atypical moles (Clarks nevi or dysplastic nevi)
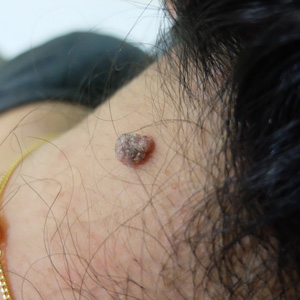
Current statistics indicate that approximately one in ten people have one or more atypical moles. An atypical mole is often larger than a common mole, and may have irregular borders that are poorly defined, possibly containing notches. The color of an atypical mole may range from light tan to dark brown, and may have a background of pink.
An atypical mole may look somewhat like a common mole, having both raised and flat portions and borders that may fade into the skin surrounding the mole.
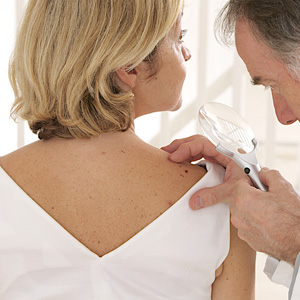
Treatment plan for Moles and Skin Cancer - Dr. Roger Koreen

Contact Dr. Roger Koreen to learn more about moles and skin cancer treatments.
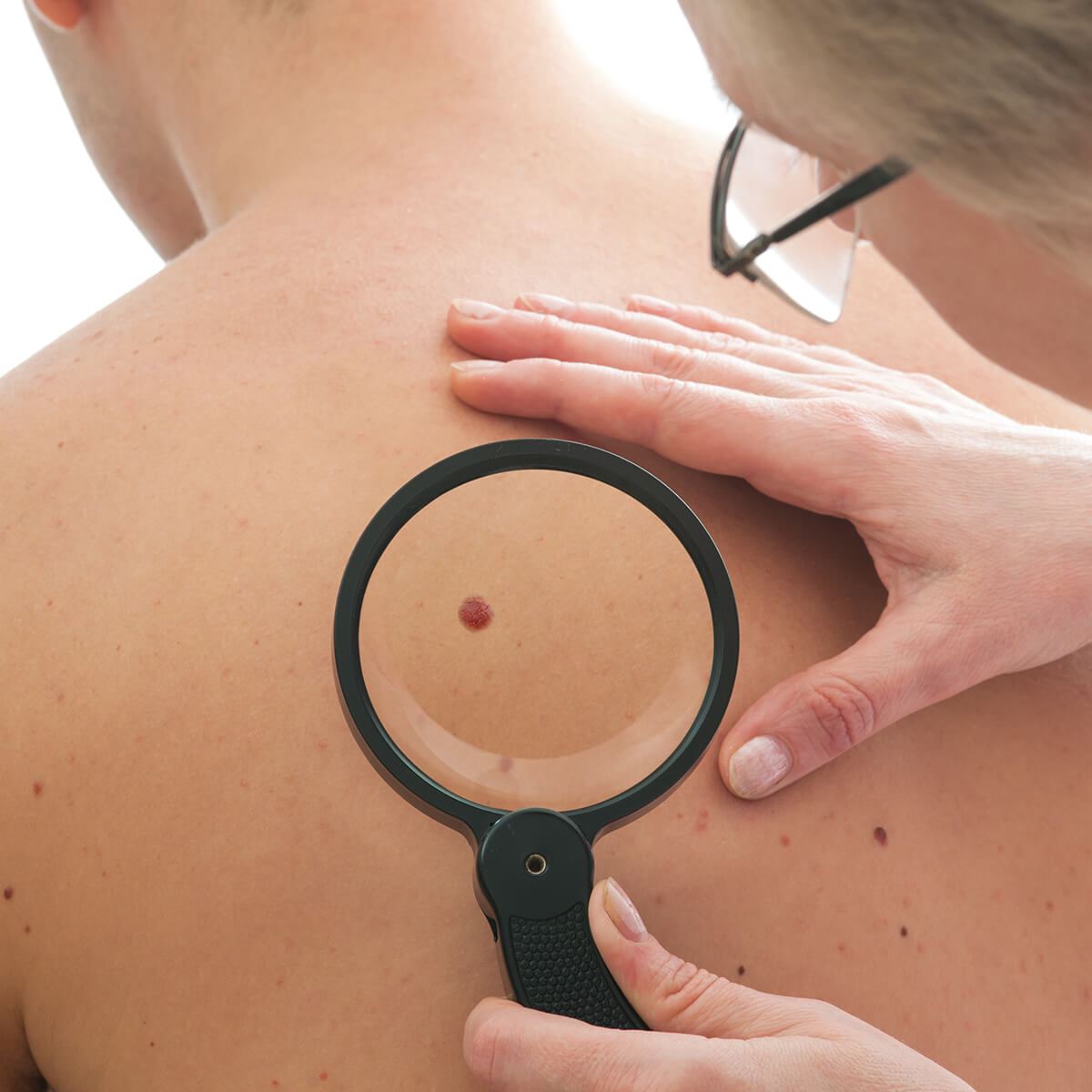
Can moles be cancerous?
A – Asymmetry (one half of the mole doesn’t match the other)
B – Border irregularity
C – Color that is not uniform
D – Diameter greater than 6mm
E – Evolving size, shape or color.
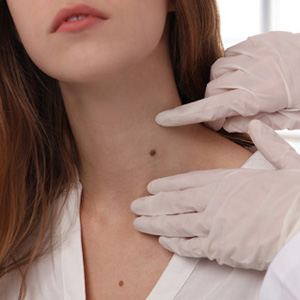
You can observe your moles and see if they follow a certain pattern, similar colour or shape.
Congenital nevi
Congenital moles are present in only about one in one-hundred infants. This type of mole may be very small, ¼ inch or less, or large enough to cover the majority of the skin on the body. In addition to size, congenital moles can also vary widely in hairiness, texture (some have a “goosebump” appearance), color, and shape. Some may appear very dark, others reddish-tan. The most common color of congenital moles is some shade of brown, which will also vary from light to dark in shade.
Larger congenital moles, of four inches or more, are present in about only every 20,000 infants. Those that cover a large portion of the body are even less common, present in one of 200,000 to 500,000 infants. Along with a very large congenital mole may also be several or hundreds of smaller moles, called “satellite” nevi. In rare instances, nevus cells may form near the brain and in the spinal cord, a condition called neurocutaneous melanosis.
Melanoma and congenital moles
Though the precise risk of melanoma development within a giant congenital mole is unknown at the time, it is estimated at no less than six percent. Melanoma within satellite nevi has not been detected, and the risk in giant congenital moles on the arms and legs is also quite small. Smaller congenital moles are more common but less risky, with malignancy before puberty a very rare occurrence. Congenital moles grow along with the body, and may change in shade from light to dark. Changes from one color to another, in shape, size, or texture, bleeding, pain, or itching are all concerning developments that should be evaluated by a skilled physician if they persist for more than a few weeks.
Treatment
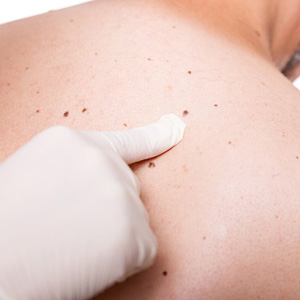
Nevi should be removed surgically when there is a reasonable concern that cancerous cells exist. Though moles may be removed for cosmetic reasons, the risk of scarring from surgical excision should be considered before this type of treatment. Smaller nevi may be removed through alternative methods, such as “shaving.” Larger moles may be excised, or cut out, in an in-office procedure.
Exceptionally large nevi may be cut out in stages in a procedure called a “serial excision.” This method allows the dermatologist to take out small portions of a mole until the entire growth is removed. The excision of a very large mole creates too large of an opening to be sutured without additional coverage. This coverage is achieved with a skin graft of split thickness, harvested from an area of the body in which skin cells are healthy. The area from which skin cells are taken may sustain scarring, and will likely be more fragile than it was prior to harvesting.
At the Dermatology and Cosmetic Laser Center of Huntington, we can help you identify abnormal nevi and treat suspicious growths. Contact us at (631) 417-3300.